Many people focus on premiums and deductibles when choosing a Medicare prescription drug plan, but the pharmacy you use can also affect how much you pay for medications.
You can fill your prescriptions at either type of pharmacy since both are considered in-network, but the cost of your medications may differ depending on which one you choose.
What Is a Preferred Pharmacy?
A preferred pharmacy is a pharmacy that has negotiated lower pricing with your prescription drug plan.
- Lower copays for certain medications
- Better overall pricing on common prescriptions
- Lower coinsurance in some stages of the plan
Preferred pharmacies can include large national chains, regional pharmacies, or even some local independent pharmacies depending on the plan.
What Is a Standard Network Pharmacy?
A standard network pharmacy is still part of your plan’s network and can fill your prescriptions.
However, these pharmacies may have:
-
Higher copays
- Slightly higher coinsurance costs
This means you can still use them, but your medication may cost more compared to a preferred pharmacy.
Can I Use Either Pharmacy?
Yes.
However, using a preferred pharmacy when possible may help reduce your out-of-pocket prescription costs. Many people continue using their regular pharmacy, especially if it is convenient. But depending on the plan and medication, it can be helpful to check whether your pharmacy is listed as preferred.
Example: Preferred vs. Standard Pharmacy Cost Difference
Below is an example using the Wellcare Value Script (PDP) plan available in Missouri. In this example we are comparing the cost of Atorvastatin, a commonly prescribed cholesterol medication.
Walmart is considered a standard network pharmacy
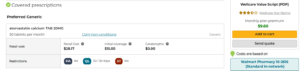
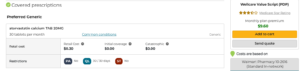
As the example above shows, the same medication can have different costs depending on the pharmacy you use. Even though both pharmacies are in-network, preferred pharmacies may offer lower copays for certain medications.
How to Check If Your Pharmacy Is Preferred?
You can usually check if your pharmacy is listed as preferred by:
- Calling member services using the phone number on the back of your prescription drug plan ID card
- Logging into your member portal to review your pharmacy network
- Visiting your carrier’s website and searching the pharmacy directory
Because pharmacy networks can change each year, it’s a good idea to confirm this during your annual Medicare plan review.


